It’s in us to give
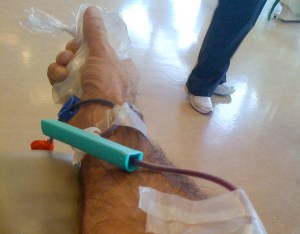
IT’S 8:10 AM on a Tuesday morning as I enter the Guelph blood donor clinic. I love this place on a sunny day like today, with its comfy recliner chairs and bright, south-facing windows – even if the primary view is a Mr. Lube auto shop. I ignore the TV that’s suspended from the ceiling, tuned to CP24 news. I prefer to watch the clinic hubbub, the other donors and the morning traffic on Silvercreek Parkway.
I’ll be out of here quickly, because I’m nearly their first customer. With half a dozen or more clinic staff (all women) just waiting to do their jobs with customary kindness and efficiency this will be a breeze. A piece of cake. It’s been awhile since I donated, over three years in fact. The intake nurse is about to explain the process as if I’m a first-timer, but then she looks again at my card which has a big grey “50” on it. This will be my 57th donation she calculates by counting the stamps on the back. She pokes my finger, takes a few drops of blood and tests them for iron levels.
I explain my absence: “I got anemic and gave it up for awhile.” I don’t go into details, but as a regular runner, giving away my red blood cells wasn’t working. “It’s like reverse blood doping,” says Deb, a running colleague, with a laugh. “You feel it immediately.”
But I came back because I miss it. I’ll be a lot more careful how often I donate now, maybe two or three times a year, or when I hear their radio ads in the summer appealing for donors.
Miss it? Yeah, I do. It’s a time out in the middle of my work week. And it’s the easiest form of voluntarism going. No committees to sit on. Very anonymous, but deeply gratifying, because of the intimacy of what you’re doing. “It’s in you to give,” is the Canadian Blood Services slogan. As a communicator often working for non-profits, I admire that persuasive brevity, an emotional appeal wrapped in a plain statement of fact.
I started giving when I was in my early 20s. It’s not something my parents or anyone I knew ever did. But the year before my first donation at university I was in a violent highway accident. I didn’t receive a blood transfusion, but I did lose something – someone close to me. Giving blood felt like payback for the fact that I was a survivor of a catastrophe, a thank you and a remembrance, a periodic reminder that life is fragile and precious, and that we depend on each other.
I didn’t really get into the routine of it until I settled, had kids and lived in my own home – in my 30s. It was still a hassle, because my rural community had only temporary clinics, set up in the local Canadian Legion hall once every quarter. When you did go, they had no reservation system, so with lineups you could spend up to two hours on your 10-minute donation. As a result, I gave maybe once or twice a year.
Back then, I donated through the Red Cross. But this was during the 1980s HIV crisis, when thousands of hemophiliacs died from “the gift of life”, the slogan of that era. As a result, the donation system changed radically and was transferred to Canadian Blood Services. It took them a few years to work out the kinks, but eventually the new rules – designed to screen out blood donors who might be carrying HIV or other blood-born disease – improved the efficiency of the system for everyone, even though it added 10–15 minutes to every visit.
When we moved to Guelph four years ago, I immediately started attending the city’s permanent clinic, which was posh compared to my years in Fergus and Elora. It was open all week long. And Canadian Blood Services cut the length of time between donations from roughly three months to two, as a way of coping with blood shortages, due (I suspect) partly to the stringent new donation procedures. That meant I could give up to six times per year, and I obliged, that is until my ferritin levels took the plunge, leaving me listless when I tried to run fast.
As much as I liked the new system for its efficiency, it turned many people off. Especially the one-on-one, closed door interview with a nurse (always female), with her 15 questions, delivered in a rapid-fire barrage that always reminds me of a spy movie interrogation (“Ven did you last see yaw fadder?”):
- Have you ever taken drugs or money for sex, even one time?
- Have you ever had sex with someone whose sexual background you didn’t know?
- Have you ever had sex with a man, even once?
I try to face the questions with a bit of humour, a nod to the element of absurdity, without smirking or letting my voice quaver. Today, my interrogator is burning through the list, even colouring in the little “no” boxes a millisecond before I answer in the negative. I’m tempted to blurt “yes” to a question about my sexual contact with people of African origin, just to throw her off. “Just kidding” I would say when she looked up from the form (we’re not making eye contact at all). But I suspect it wouldn’t go over very well, like joking about weapons when you’re in the airport security lineup.
The nurse inspects my forearms for needle marks (signs of intravenous drug use), then takes my blood pressure, temperature and heart rate, all normal. After all this prep, and despite the fact that my blood will be lab tested for HIV and several other diseases, CBS still has a back-up plan, in case you’re lying, and giving blood for appearance’s sake (like, for example, so your wife doesn’t suspect that you’ve been having anonymous sex with men in parks all your adult life). They have a secret weapon, a last resort, which will silently torpedo your donation, removing it from the blood supply at the lab.
Here’s how it works. The nurse leaves the room after handing you a sheet with two tiny, stick-on bar codes. One means “use my blood”, the other “do not use my blood.” The sheet says to ask yourself, “Do I believe my blood is safe to give to a person I really care for?” You answer by sticking one of the bar codes in a box at the bottom of your donation form. The system provides anonymity even to the nurse who just asked you all those shockingly personal questions. It allows you to be a fake donor, if you so desire – an accommodation to the complexities of human society, yet one that preserves the safety of the donation system.
By 8:30 I’m through the screening process, heading for a a right-side donation chair (most donors have a favourite, one arm that just works better than the other). I chat with the nurse, Anna, who is pleasant, polite, and likes to talk about more than the dastardly snowfall we had on the weekend.
“What do you do for a living, if I may ask?” she inquires, even as she rigorously times the disinfection of my arm and the assembly of the plastic donation bags.
“I’m a graphic designer,” I reply.
“Oh, I could tell by your glasses that were something artsy,” she says with a smile. Snap goes the little sheath covering the sterile needle. “I like artsy – don’t get a lot of it in this job, which is all about rules and procedure.”
Very quickly, Anna slips the needle into my bulging vein, and I can hear the gentle rocking of the collection machine that sits on the floor below me. But almost immediately there’s a problem. Anna stops chatting. A red warning light is flashing on her machine, signifying low blood flow, which can lead to coagulation. She asks me to pump my fist; thankfully, the green light returns. She looks relieved, and goes to serve the other donors now arriving.
But my arm doesn’t feel great. Usually, I’m nearly unaware of the donation as it happens. Today, I can literally feel the needle in my vein and its mild pressure. I try not to focus on it. Anna returns, with a colleague, who gives me a concerned look. They bring a warm cloth in a plastic bag and ask me to squeeze it. “Not too hard,” they say, “that might push the needle out.” Really gals, I’m trying not to think about the needle here.
They leave, but a third nurse comes over, removes the adhesive tape and begins to adjust the needle, very gently of course, but it hurts. My mouth goes very dry. There’s a slight pounding in my ears. I sit quietly for a few seconds, then meet her eyes: “You have to take that out,” I say emphatically. She responds immediately – in a few seconds I’m free of the needle, holding a compress to my vein.
Anna returns. “Can I have a glass of water?” I ask immediately. Instead of obliging me, she asks questions. “How do you feel?” (Okay.) “Can you hear my voice normally?” (Yes.)
“Do you feel faint or nauseous?” I answer “no” to the last question and she turns to walk away, so I correct myself quickly: “YES!”
Anna gives some sort of secret signal to the other clinic staffers and suddenly I’ve got three nurses around me. The place has lost its gentle morning calm; the other donors are peering over at my station, wondering why I’ve suddenly got so much attention. Anna tilts my chair back until my feet are well above my head, and they quickly place cold wet cloths on my forehead and behind my neck. They take my blood pressure, which confirms the obvious: it is low. The remedial measures aren’t helping. I feel like there’s a train bearing down at me and I’m stuck on the tracks.
“How do you feel, on a scale of 0 to 10?” asks Anna.
“Three?” I reply weakly, then repeat my plea: “Can I have some water, or juice?”
Anna returns with a small carton of apple juice, but won’t give it to me just yet. If I go under, they don’t want fluid in my mouth. But it’s a a catch-22 because it seems like the only thing that will revive me now. I’m struggling, slipping, falling.
For maybe five minutes I’m on a knife-edge, normalcy on one side and a black void on the other. I’ve fainted before, almost half a dozen times, although never while giving blood. In my early 40s, after a morning faint that involved a particularly harsh collision with a bathtub and stitches to my head, my doctor finally sent me for a “tilt table test” in Hamilton. There, they simulated a faint by forcing me to stand immobile for 30 minutes while they monitored my heart and blood pressure.
It worked – I fainted (at which point they tilted the table I was strapped to from vertical back to horizontal, hence the name of the test). It confirmed that I’m a normal vaso-vagal fainter: blood pooling in the legs, falling blood pressure, abrupt change in heart rate, etc., etc. For me, the causes are now familiar and the clincher is usually some sort of internal pain, an abdominal cramp, a sprained ankle … or a wonky blood donation needle.
Fainting is a curious mix of the body and the mind, however. My first one happened as I sat at the breakfast table, reading a magazine account of the rowing accident that nearly cost Silken Laumann her leg and her Olympic career. I read: “The German boat collided with Laumann’s, its sharp bow shearing her calf muscle away from the bone … ” Next thing I knew, I was on the floor. (Laumann famously won Olympic bronze for Canada in Barcelona, just 10 weeks after that accident.)
This time, I’m already horizontal, but still feel like I’m still about to get sucked under. When I tell my wife about it later, she asks, “Isn’t it like trying to stifle a sneeze? Wouldn’t it be better if you just fainted?” I can’t describe to her the dread and the fear that accompanies the fainting urge. I know it’s harmless, but it feels ghastly. And afterwards, the disorientation is acute. I resist with the only tactics available, breathing deeply and erasing the needle thing from my thoughts.
Finally, Anna relents and gives me a sip of the apple juice. I tell her I’m a 5. She lets me hold the box. I drain it and she gets me another. It’s an elixir. I ask for a third one. “I’m a 7,” I promise her with a wink.
By 9:30 am I’m able to walk out of the clinic and drive myself back to work, after all trace of the sensation is gone and my colouring is normal. My last question to Anna as I leave the clinic is about my bag of blood. I expected it would be useless, since the donation was aborted early. But I’d seen the phlebotomists agitating and packaging it for shipment as I recovered. She confirms that I gave just enough (they weigh the bag), roughly 500 ml or 10 percent of my blood volume.
“So this wasn’t all in vein?” I ask her, attempting a pun. “No, it wasn’t in vain,” she replies. “Thank you, and come again soon.”


